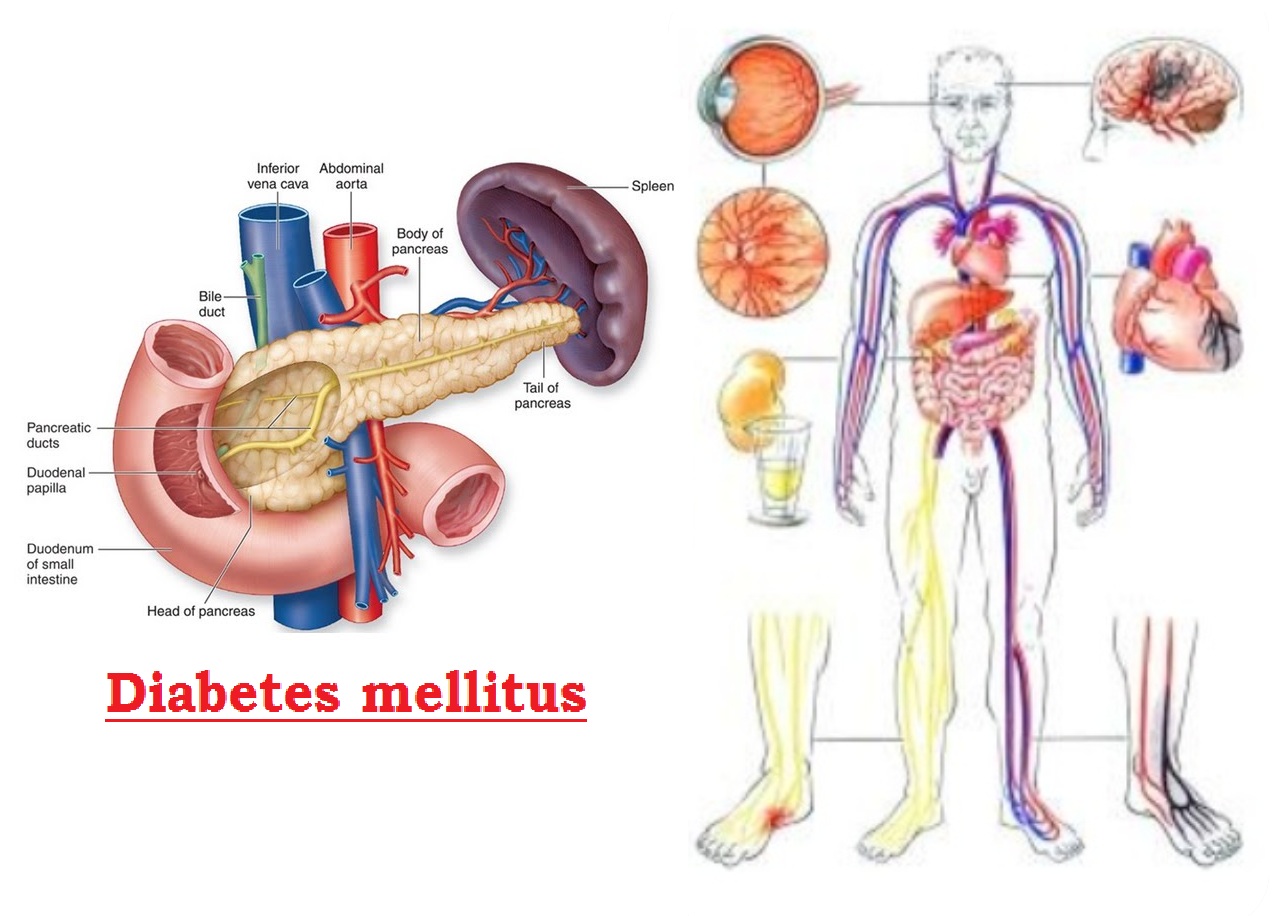
Diabetes mellitus is a chronic metabolic syndrome characterized as Polyuria, Polydipsia & polyphagia caused by hyperglycemia due to absolute or relative deficiency of insulin. Deficiency of insulin affects the metabolism of carbohydrate, protein and fat, and can cause a significant disturbance of water and electrolyte homeostasis. Glucose is vital to human health because it's an important source of energy for the cells that make up muscles and tissues. It's also human brain's main source of fuel. If the person have diabetes mellitus, no matter what type, it means person have too much glucose in the blood circulation, although the causes may differ. Too much glucose can lead to serious health problems. Chronic diabetes mellitus includes Type-I diabetes mellitus and Type-II diabetes mellitus. Potentially reversible diabetes mellitus include prediabetes ; when blood sugar levels are higher than normal, but not high enough to be classified as diabetes; and gestational diabetes, which occurs during pregnancy but may resolve after the delivery. Diabetes is a major cause of blindness, kidney failure, heart attacks, stroke and lower limb amputation.
The number of people with Diabetes mellitus has risen from 108 million in 1980 to 422 million in 2014 worldwide. The global prevalence of Diabetes mellitus among adults over 18 years of age has risen from 4.7% in 1980 to 8.5% in 2014. Diabetes prevalence has been rising more rapidly in middle- and low-income countries. In 2016, an estimated 1.6 million deaths were directly caused by Diabetes mellitus. Another 2.2 million deaths were attributable to hyperglycemia in 2012. Almost half of all deaths attributable to high blood glucose occur before the age of 70 years. WHO estimates that diabetes was the seventh leading cause of death in 2016. India is one of the 6 countries of the IDF SEA region. About 425 million people have diabetes mellitus in the world and 82 million people in the SEA Region; by 2045 this will rise to 151 million. There were over 72.946.400 cases of diabetes in India in 2017.
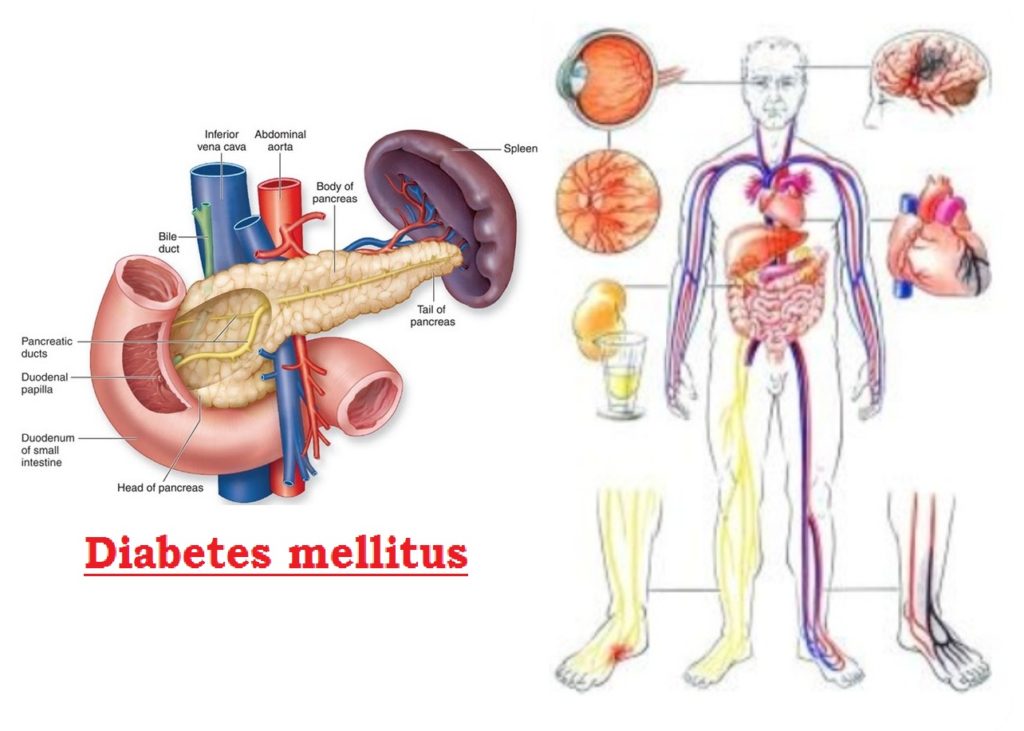
Sign & Symptoms :
The sign & symptoms of diabetes mellitus are depending on how much blood glucose is elevated. Some people, especially those with prediabetes or Type-II diabetes, may not experience symptoms initially. In Type-I diabetes, symptoms tend to come on quickly and be more severe. Death may result from acute metabolic decompensation, while long-standing metabolic derangement is frequently
associated with functional and structural changes in the cells of the body, with those of the vascular system being particularly susceptible. These changes lead to the development of clinical 'complications' of diabetes which characteristically affect the eye, the kidney and the nervous system. Some of the common signs and symptoms of Type-I and Type-II diabetes mellitus are as follows:
- Polydipsia (Increased thirst)
- Polyuria (Frequent urination)
- Polyphagia (Extreme hunger)
- Unexplained weight loss
- Presence of ketone bodies in the urine (ketones are a byproduct of the breakdown of muscle and fat that happens when there's not enough available insulin)
- Fatigue
- Irritability
- Blurred vision
- Slow-healing sores
- Frequent infections, such as gums or skin infections and vaginal infections
Although Type-I diabetes can develop at any age, it typically appears during childhood or adolescence. Type-II diabetes, the more common type, can develop at any age, though it's more common
in people older than 40 years.
Causes of Diabetes mellitus :
The causes of diabetes mellitus are depends of several factors relating to utilization of blood glucose in the human body. To understand diabetes mellitus, firstly understand how glucose is normally digested, absorbed and metabolized in the body.
Insulin is a hormone that secreted from the β-cell of islets of Langerhans of the pancreas situated behind and below the stomach. The pancreas secretes insulin into the bloodstream and circulates, enabling glucose to enter cells. Insulin lowers the amount of glucose in the bloodstream.
Glucose is a source of energy for the cells that make up muscles and other tissues. Glucose comes from two major sources: food and liver. Sugar is absorbed into the bloodstream, where it enters into the cells with the help of insulin. When blood glucose levels are low, such as when glucose haven't eaten in a while, the liver breaks down stored glycogen into glucose to keep blood glucose level within a normal range.
Causes of Type-I Diabetes mellitus :
The exact cause of Type-I diabetes is unknown. Type-I diabetes also known as juvenile diabetes or insulin-dependent diabetes, is a acute condition in which the pancreas produces very low amount of insulin or complete cessation of insulin secretion. Human immune system ; which normally fights against harmful bacteria or viruses by attack and unfortunately this destroys insulin-producing cells in
the pancreas. Insulin is a hormone needed to allow sugar (glucose) to enter into the cells to produce energy. Different factors, including genetics and some viruses, may contribute to type 1 diabetes. Although type 1 diabetes usually appears during childhood or adolescence, it can develop in adults. Actually, Type-I diabetes mellitus has no cure. Treatment focuses on managing blood glucose levels with insulin, diet control and lifestyle management to prevent complications. Type-I is thought to be caused by a combination of genetic susceptibility and environmental factors, though exactly what many of those factors are is still unclear.
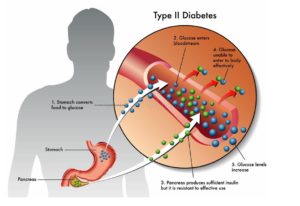
Causes of Prediabetes and Type-II Diabetes mellitus :
In case of prediabetes, which can lead to Type-II diabetes mellitus and in Type-II diabetes mellitus, cells become resistant to the action of insulin, and/or the pancreas is unable to make enough amount of insulin to overcome this resistance; Instead of moving into cells where it's needed for energy, glucose builds up in the bloodstream. Some common causes of Type-I diabetes mellitus are Being overweight, eating a lot of foods, drinks or with sugar and simple carbohydrates, artificial sweeteners (sugar free sodas, sugar free foods) intake, Lack of activity (sedentary behavior), Lack of exercise, stress and stress hormones and some genetics problems. Exactly why this happens is uncertain, although it's believed that genetic and environmental factors play a role in the development of Type-II diabetes. Being overweight is strongly linked to the development of Type-II diabetes, but not everyone with Type-II is overweight.
Causes of Gestational Diabetes mellitus :
During pregnancy, the placenta produces hormones to sustain pregnancy. These hormones make cells more resistant to insulin. Normally, the pancreas responds by producing enough extra
insulin to overcome this resistance. But sometimes pancreas can't keep up. When this happens, too little glucose gets into cells and too much stays in the bloodstream, resulting in gestational diabetes. When carbohydrate intolerance is noticed for a first time during pregnancy this is known as Gestational Diabetes mellitus (GDM). Here, fasting glucose level is >126 gm/dl and they are more susceptible for development of frank diabetes mellitus.
Diagnosis of Diabetes mellitus :
Symptoms of Type-I diabetes mellitus often appear suddenly and are often the reason for checking blood sugar levels. Because symptoms of other types of diabetes and prediabetes come on more gradually or may not be evident, the American Diabetes Association (ADA) has recommended screening guidelines. The ADA recommends that the following people be screened for diabetes mellitus :
- Anyone with a body mass index [BMI=Body weight (kg)/Height2 (h2)] higher than 25, regardless of age, who has additional risk factors, such as high blood pressure, a sedentary lifestyle, a history of polycystic ovary syndrome, having delivered a baby who weighed more than 9 pounds, a history of diabetes in pregnancy, high cholesterol levels, a history of heart disease and having a close relative with diabetes mellitus.
- Anyone older than age 45 is advised to receive an initial blood sugar screening and then, if the results are normal, to be screened every three years thereafter.
Tests for Type-I and Type-II Diabetes mellitus & prediabetes :
- Glycated hemoglobin (HbA1C) test : Glycated hemoglobin or Glycosylated hemoglobin (HbA1C) blood test indicates average blood sugar level for the past three months. It measures
the percentage of blood glucose attached to hemoglobin; the oxygen-carrying protein in red blood cells. The higher blood sugar levels, the more hemoglobin attached with free glucose. An HbA1C level of 6.5 percent or higher on two separate tests indicates that the person have propensity to diabetes mellitus. An HBA1C between 5.7 and 6.4 percent indicates prediabetes. Below 5.7 is considered normal. If the HBA1C test results aren't consistent, the test isn't available, or if the person have certain conditions that can make the HbA1C test inaccurate such as if the person're pregnant or have an uncommon form of hemoglobin (known as a hemoglobin variant) - Random blood sugar test : A blood sample will be taken at a random time. Regardless of when the person last ate, a random blood glucose level of 200 mg/dl or higher suggests diabetes mellitus.
- Fasting blood sugar test : A blood sample will be taken after an overnight fast. A fasting blood sugar level less than 110 mg/dl is normal. A fasting blood glucose level from 110 to 125 mg/dl
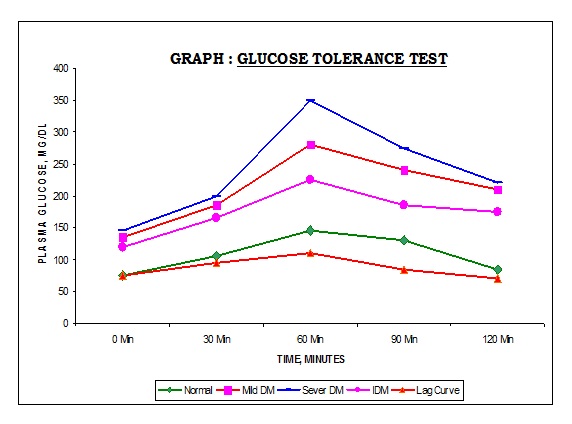
is considered prediabetes. If it's 126 mg/dL (7 mmol/L) or higher on two separate tests, the person have diabetes mellitus. - Oral glucose tolerance test (OGTT) : For this test, patient have fast overnight, and the fasting blood sugar level is measured. Then he/she drink 75 -100 mg of anhydrous glucose (1.75 gm/Kg weight) dissolved in 250-300 ml of water and blood glucose levels are measured periodically for the next two hours. A blood sugar level less than 140 mg/dl (7.8 mmol/L) is normal. A reading of more than 200 mg/dl (11.1 mmol/L) after two hours indicates diabetes mellitus. A reading between 140 mg/dl and 199 mg/dl (7.8 mmol/L and 11.0 mmol/L) indicates prediabetes.
Type-I diabetes mellitus suspected case :
Urine will be tested to look for the presence of a byproduct (ketonebodies); produced when muscle and fat tissue are used for energy but the body doesn't have enough insulin to use the available glucose.
Tests for gestational diabetes :
Doctor will be evaluate risk factors for gestational diabetes if pregnant mother have an early history in her previous pregnancy. If She is at high risk of gestational diabetes - for example, if she was obese at the start of her pregnancy, She had gestational diabetes during a previous pregnancy, or she has a mother, father, sibling or child with diabetes , then doctor may test for diabetic profile at first prenatal visit. If she is at average risk of gestational diabetes, She'll likely have a screening test for gestational diabetes during her second trimester (in between 24 and 28 weeks of pregnancy). Doctor may use the following screening tests:
- Initial glucose challenge test : She'll begin the glucose challenge test by drinking a syrupy glucose solution. One hour later, She'll have a blood test to measure her blood glucose level. A blood glucose level below 140 mg/dl (7.2 to 7.8 mmol/L) is usually considered normal on a glucose challenge test. If her blood glucose level is higher than normal, it only means she has a higher risk of gestational diabetes. Then doctor will order a follow-up test to determine gestational diabetes.
- Follow-up glucose tolerance test : For the follow-up test, She'll be asked to fast overnight (fasting for about 10-12 hours) and then given blood sample for measurement of fasting plasma glucose level. Afterwards she'll drink 75 -100 mg of anhydrous glucose (1.75 gm/Kg weight) dissolved in 250-300 ml of water and blood glucose levels are measured periodically in the interval of one hour for the next two hours . If at least two of the blood glucose level readings are higher than the normal values established for each of the three test, She'll be diagnosed with gestational diabetes.
Complications of Diabetes mellitus :
Long term complications of diabetes mellitus develop gradually. The severity of complication depends on how much longer period patient have diabetes and how much controlled blood glucose level.
Eventually, diabetes mellitus complications may be disabling or even life-threatening. Possible complications include:
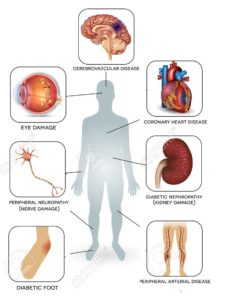
- Cardiovascular disease : Diabetes mellitus dramatically increases the risk of various cardiovascular problems, including coronary artery disease with chest pain (angina), heart attack, stroke and
narrowing of arteries (atherosclerosis). If the patient have diabetes then he/she are more likely to have heart disease or stroke. - Nerve damage (neuropathy) : Excess sugar can injure the walls of the tiny blood vessels (capillaries) that nourish nerves, especially in the legs. This can cause tingling, numbness, burning or
pain that usually begins at the tips of the toes or fingers and gradually spreads upward. Left untreated, patient could lose all sense of feeling in the affected limbs. Damage to the nerves related to digestion can cause problems with nausea, vomiting, diarrhea or constipation. For men, it may lead to erectile dysfunction. Nerve damage in the feet or poor blood flow to the feet, increases
the risk of various foot complications. Left untreated, cuts and blisters can develop serious infections, which often heal poorly. These infections may ultimately require toe, foot or leg amputation. - Kidney damage (nephropathy) : The kidneys contain millions of tiny blood vessel clusters (glomeruli) that filter waste product of the body from blood. Diabetes mellitus can damage
this delicate filtering system. Severe damage can lead to kidney failure or irreversible end-stage kidney disease, which may require dialysis or a kidney transplant. - Eye damage (retinopathy) : Diabetes can damage the blood vessels of the retina (diabetic retinopathy), potentially leading to blindness. Diabetes also increases the risk of other serious vision
conditions, such as cataracts and glaucoma. - Skin infection : Diabetes may leave the patient more susceptible to skin problems, including bacterial and fungal infections.
- Hearing impairment : Hearing problems are more common in people with diabetes mellitus.
- Alzheimer's disease : Type-II diabetes mellitus may increase the risk of Alzheimer's disease. The poorer blood glucose control, greater the risk appears to be. Although there are
theories as to how these disorders might be connected, none has yet been proved.
Complications of gestational Diabetes mellitus :
Most women who have gestational diabetes deliver healthy babies. However, untreated or uncontrolled blood glucose levels can cause problems for both mother and her baby.
Complications in baby can occur as a result of gestational diabetes includes:
- Excess growth : Extra glucose can cross the placenta, which triggers baby's pancreas to make extra insulin. This can cause, baby to grow too large (macrosomia). Very large babies
are more likely to require a C-section birth. - Low blood glucose level : Sometimes babies of mothers with gestational diabetes develop low blood sugar (hypoglycemia) shortly after birth because their own insulin production is
high. Prompt feedings and sometimes an intravenous glucose solution can return the baby's blood sugar level to normal. - Type-II diabetes mellitus later in life : Babies of mothers who have gestational diabetes have a higher risk of developing obesity and Type-II diabetes later in life.
- Death : Untreated gestational diabetes can result in a baby's death either before or shortly after birth.
Complications in the mother can occur as a result of gestational diabetes includes :
- Preeclampsia : This condition is characterized by high blood pressure, excess protein in the urine and swelling in the legs and feet. Preeclampsia can lead to serious or even
life-threatening complications for both mother and baby. - Subsequent gestational Diabetes mellitus : Once mother have had gestational diabetes in one pregnancy, she is more likely to have it again with the next pregnancy. Mother're
also more likely to develop diabetes; typically Type-II diabetes.
Treatment of Diabetes mellitus :
Treatment of the patient is depending on the type of diabetes mellitus patient have. Blood glucose level monitoring, insulin and oral medications may play a major role in diabetes treatment. Eating a healthy diet, maintaining a healthy weight and participating in regular activity also are important factors for managing diabetes.
Treatments for all types of diabetes :
An important part of managing diabetes mellitus as well as patient overall health and weight depends on through a healthy diet and exercise plan:
- Healthy diet : Contrary to popular perception, there's no specific diabetes diet. Patient will need to center his/her diet on more fruits, vegetables and whole grains ; foods that are high in nutrition and fiber and low in fat and calories and cut down on animal products, refined carbohydrates and sweets. In fact, it's the best eating plan for the entire family. Sugary foods are OK once in a while, as long as they're counted as part of meal plan. Yet understanding what and how much to eat can be a challenge. A registered dietitian can helps to create a meal plan that fits for patient's health goals, food preferences and lifestyle. This will likely include carbohydrate counting, especially if the person have Type-I diabetes.
- Physical activity : Everyone needs regular aerobic exercise and people who have diabetes are no exception. Exercise lowers your blood sugar level by moving glucose into the cells, where
it's used for energy. Exercise also increases sensitivity to insulin, which means body needs less insulin to transport sugar to the cells. Always choose enjoyable activities, such as walking, swimming or biking. What's most important is making physical activity part of the daily routine. Aim for at least 30 minutes or more of aerobic exercise most days of the week. If patient haven't been active for a while, start slowly and build up gradually.
Treatments for Type-I and Type-II Diabetes mellitus :
Treatment for Type-I diabetes involves insulin injections or the use of an insulin pump, frequent blood sugar checks, and carbohydrate counting. Treatment of Type-II diabetes primarily involves monitoring of blood sugar, along with diabetes medications, insulin or both.
- Monitoring blood sugar level : Depending on treatment plan, patient may check and record his/her blood sugar as often as several times a week to as many as four to eight times a day. Careful monitoring is the only way to make sure that the blood sugar level remains within target range. People who receive insulin therapy also may choose to monitor their blood sugar levels with a continuous glucose monitor. Although this technology doesn't yet replace the glucose meter, it can provide important information about trends in blood glucose levels. Even with careful management, blood sugar levels can sometimes change unpredictably. With the help from diabetes treatment team, learn how blood sugar level changes in response to food, physical activity, medications, illness, alcohol, stress (for women, fluctuations in hormone levels). In addition to daily blood sugar monitoring, doctor will likely recommend regular HbA1C testing to measure average blood sugar level for the past two to three months. Compared with repeated daily blood sugar tests, Hb A1C testing better indicates how well diabetes treatment plan is working overall. An elevated HbA1C level may signal the need for a change in insulin regimen or meal plan. Targeted HbA1C goal may vary depending on the age and various other factors of the patients. However, for most people with diabetes, the American Diabetes Association recommends an HbA1C of below 7 percent.
- Insulin therapy : People with Type-I diabetes need insulin therapy to survive. Many people with Type-II diabetes or gestational diabetes also need insulin therapy. Many types of insulin are available, including rapid-acting insulin, long-acting insulin and intermediate options. Depending on your needs, your doctor may prescribe a mixture of insulin types to use throughout the day and night. Insulin can't be taken orally to lower blood sugar because stomach enzymes interfere with insulin's action. Often insulin is injected using a fine needle and syringe or an insulin pen (a device that looks like a large ink pen). An insulin pump may also be an option. The pump is a device about the size of a cellphone worn on the outside of your body. A tube connects the reservoir of insulin to a catheter that's inserted under the skin of abdomen. A tubeless pump that works wirelessly is also now available. Always program an insulin pump to dispense specific amounts of insulin. It can be adjusted to deliver more or less insulin depending on meals, activity level and blood sugar level.
- Artificial pancreas : An emerging treatment approach, not yet available, is closed loop insulin delivery, also known as the artificial pancreas. It links a continuous glucose monitor to an insulin pump. The device automatically delivers the correct amount of insulin when the monitor indicates the need for it. There are a number of different versions of the artificial pancreas, and clinical trials have had encouraging results. More research needs to be done before a fully functional artificial pancreas can receive regulatory approval. However, the first step toward an artificial pancreas was approved in 2013. Combining a continuous glucose monitor with an insulin pump, this system stops insulin delivery when blood sugar levels drop too low. Studies on the device found that it could prevent low blood sugar levels overnight without significantly increasing morning blood sugar levels.
- Oral or other medications : Sometimes other oral or injected medications are prescribed as well. Some diabetes medications stimulate pancreas to produce and release more insulin. Others inhibit the production and release of glucose from liver, which means, need less insulin to transport sugar into the cells. Still others block the action of stomach or intestinal enzymes that break down carbohydrates or make tissues more sensitive to insulin. Metformin (Glucophage, Glumetza, others) is generally the first medication prescribed for Type-II diabetes.
- Pancreas Transplantation : In some people who have Type-I diabetes, a pancreas transplant may be an option. Islet transplants are being studied as well. With a successful pancreas transplant, patient would no longer need insulin therapy. But transplants aren't always successful and these procedures pose serious risks. Person need a lifetime of immune-suppressing drugs to prevent organ rejection. These drugs can have serious side effects, including a high risk of infection, organ injury and cancer. Because the side effects can be more dangerous than the diabetes, transplants are usually reserved for people whose diabetes can't be controlled or those who also need a kidney transplant.
- Bariatric surgery : Although it is not specifically considered a treatment for Type-II diabetes mellitus, people with Type-II DM who also have a body mass index higher than 35 may benefit from this type of surgery. People who've undergone gastric bypass have seen significant improvements in their blood sugar levels. However, this procedure's long-term risks and benefits for Type-II diabetes aren't yet known.
Treatment for Gestational Diabetes mellitus :
Controlling mother blood sugar level is essential to keeping baby's healthy and avoiding complications during delivery. In addition to maintaining a healthy diet, exercising and treatment plan may include monitoring blood glucose level and in some cases, using insulin or oral medications.
Healthcare provider will also monitor blood sugar level during labor. If blood sugar rises; baby may release high levels of insulin which can lead to low blood sugar right after birth.
Control & Prevention of Diabetes mellitus :
If the person have prediabetes, healthy lifestyle choices can help him bring his/her blood sugar level back to normal or at least keep it from rising toward the levels seen in Type-II diabetes. Maintaining a healthy weight through exercise and healthy dieting can help. Exercising at least 150 minutes a week and losing 5 to 10 percent of body weight may prevent or delay Type-II diabetes.
Sometimes medications, such as metformin (Glucophage, Glumetza, others) also are an option if the person are at high risk of diabetes, including when prediabetes is worsening or if he/she have cardiovascular disease, fatty liver disease or polycystic ovary syndrome.
In other cases, medications to control cholesterol- statins, in particular and high blood pressure medications are needed. Always doctor might prescribe low-dose aspirin therapy to help prevent
cardiovascular disease in case of high risk. Healthy lifestyle choices remain key, however.
Type-I Diabetes mellitus can't be prevented. However, the same healthy lifestyle choices that help treat prediabetes, Type-II diabetes and gestational diabetes can also help prevent them:

- Eat healthy foods, Choose foods lower in fat and calories and higher in fiber. Focus on fruits, vegetables and whole grains. Strive for variety to prevent boredom.
- Get more physical activity, Aim for 30 minutes of moderate physical activity per day. Take a brisk daily walk, Ride bicycle, Swim laps. If person can't fit in a long workout, break it up into smaller sessions spread throughout the day.
- Lose excess weight, If overweight, losing even 7 percent of body weight for example, 14 pounds (6.4 kilograms) if weigh 200 pounds (90.9 kilograms) can reduce the risk of diabetes. To keep weight in a healthy range, focus on permanent changes to eating and exercise habits. Motivate yourself by remembering the benefits of losing weight, such as a healthier heart, more energy and improved self-esteem.
- Sometimes medication is an option as well. Oral diabetes drugs such as metformin (Glucophage, Glumetza, others) may reduce the risk of Type-II diabetes but healthy lifestyle choices
remain essential. - Have blood sugar checked at least once a year to check that the person haven't developed Type-II diabetes.
Healthy diet, regular physical activity, maintaining a normal body weight and avoiding tobacco use are ways to prevent or delay the onset of Type-II Diabetes mellitus. Diabetes can be treated and its consequences avoided or delayed with diet, physical activity, medication and regular screening and treatment for complications.