Multisystem Inflammatory Syndrome in Children (MIS-C), also called Pediatric Multi-system Inflammatory Syndrome (PMIS or PIMS) is a serious condition where different body parts of the children can become inflamed such as the heart, blood vessels, lungs, kidneys, gastrointestinal organs, brain, skin ear & eyes characterized by fever and various symptoms, including abdominal (gut) pain, vomiting, diarrhea, neck pain, rash, bloodshot eyes, or feeling extra tired.
The cause of MIS-C is not yet fully understood. Some researchers suspect that MIS-C is caused by a delayed immune response to the Corona virus (COVID-19) that somehow goes into overdrive, causing inflammation that damages organs. It’s also possible that the antibodies children make to the virus are creating the immune reaction. Since only a small number of children develop MIS-C, it is possible that there are genetic factors that make some children susceptible. It is important to remember that overall, children fare very well with COVID-19 as compared to adults. Only a small number of children seem to develop signs and symptoms of MIS-C, and most have recovered quickly.
 Recently, reports from Europe and North America have described clusters of children and adolescents requiring admission to intensive care units with a multisystem inflammatory condition with some features similar to those of Kawasaki disease and Toxic shock syndrome. Case reports and small series have described a presentation of acute illness accompanied by a Hyperinflammatory syndrome, leading to multiorgan failure and shock. Initial hypotheses are that this syndrome may be related to COVID-19 based on initial laboratory testing showing positive serology in a majority of patients. Children have been treated with anti-inflammatory treatment, including parenteral immunoglobulin and steroids.
Recently, reports from Europe and North America have described clusters of children and adolescents requiring admission to intensive care units with a multisystem inflammatory condition with some features similar to those of Kawasaki disease and Toxic shock syndrome. Case reports and small series have described a presentation of acute illness accompanied by a Hyperinflammatory syndrome, leading to multiorgan failure and shock. Initial hypotheses are that this syndrome may be related to COVID-19 based on initial laboratory testing showing positive serology in a majority of patients. Children have been treated with anti-inflammatory treatment, including parenteral immunoglobulin and steroids.
It is essential to characterize this syndrome and its risk factors, to understand causality, and describe treatment interventions. It is not yet clear the full spectrum of disease, and whether the geographical distribution in Europe and North America reflects a true pattern, or if the condition has simply not been recognized elsewhere.
World Health Organization has developed a preliminary case definition and case report form for multisystem inflammatory disorder in children and adolescents based on the standardized data describing clinical presentations, severity, outcomes, and epidemiology. The preliminary case definition reflects the clinical and laboratory features observed in children reported to date, and serves to identify suspected or confirmed cases both for the purpose of providing treatment and for provisional reporting and surveillance. The case definition will be revised as more data become available.
Sign & Symptoms of MIS-C :
Because the illness is so new, symptoms are still being documented, and they may vary from child to child. The main thing to watch for is a persistent fever (lasting more than 24 hours and usually present for several days), child appearing fatigued and ill, or loss of appetite or not drinking enough fluids. Some of the suspected specific features of MIS-C may includes:
- Kawasaki-like symptoms: Rash, bloodshot eyes, swollen hands and feet, cracked lips, a swollen tongue that looks like a strawberry, and an enlarged lymph node in the neck.
- Toxic shock-like symptoms: Severe flu-like symptoms with high fever, as well as a sunburn-like rash, low blood pressure, and a very high heart rate.
- Gastrointestinal symptoms: diarrhea, vomiting, abdominal pain, or a swollen abdomen.
- Respiratory symptoms: Respiratory symptoms have been reported with COVID-19, such as persistent cough and shortness of breath, may or may not be present.
- Fever >38.0°C for ≥24 hours, or report of subjective fever lasting ≥24 hours with feeling unusually tired.
- Cytokine storm/macrophage activation or hyper inflammatory features.
- Abnormal clotting, poor heart function, diarrhea and gastrointestinal symptoms, acute kidney injury.
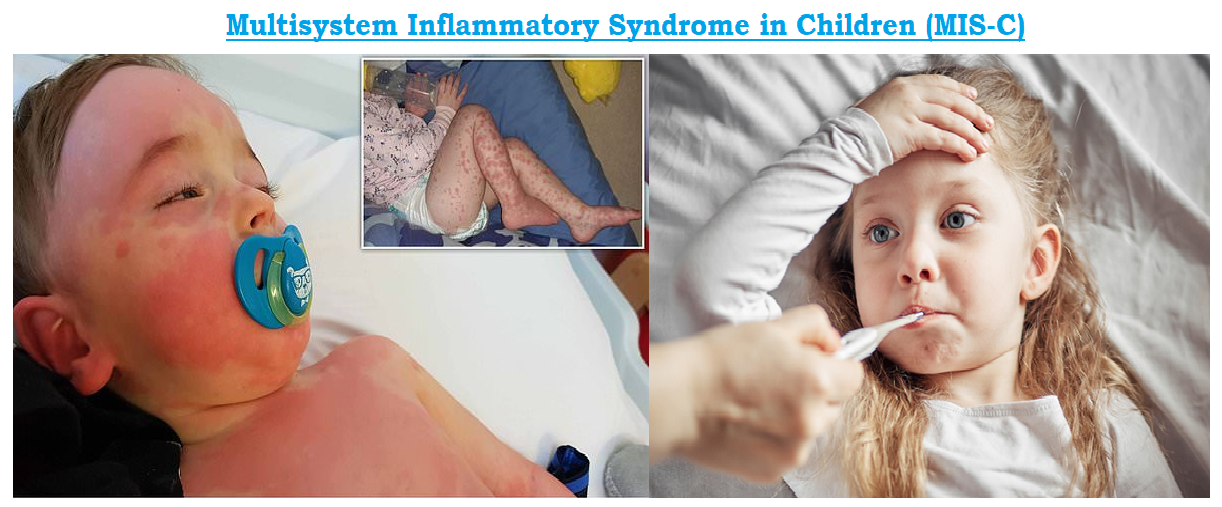 Emergency warning signs of MIS-C includes Trouble breathing, Pain or pressure in the chest that does not go away, New confusion, Inability to wake or stay awake, Bluish lips or face and severe abdominal pain.
Emergency warning signs of MIS-C includes Trouble breathing, Pain or pressure in the chest that does not go away, New confusion, Inability to wake or stay awake, Bluish lips or face and severe abdominal pain.
Diagnosis of MIS-C :
Currently, MIS-C is diagnosed based on the patient’s history and symptoms like persistent fever and dysfunction of one or more organs such as the heart, lungs or kidneys, together with laboratory tests to look for signs of inflammation in the body. Children should also have a positive test for COVID-19 or have been exposed to the virus within the past four weeks, although neither is absolutely necessary to make a diagnosis. Testing is also done to rule out other possible causes of the symptoms, such as other infections. Doctors may do certain tests to look for inflammation or other signs of disease. These tests might include:
Laboratory Testing :
- An elevated C-reactive protein (CRP), Erythrocyte Sedimentation Rate (ESR), Fibrinogen, Procalcitonin, d-dimer,Ferritin, Lactic acid dehydrogenase (LDH), or Interleukin 6 (IL-6), elevated Neutrophil , reduced Lymphocytes and low albumin.
- Similarly, SARS-CoV-2 detection by RT-PCR or antigen test is indicated.
- Where feasible, SARS-CoV-2 serology testing is suggested, even in the presence of positive RT-PCR or antigen testing. Any serology testing should be performed prior to administering IVIG or any other exogenous antibody treatments.
Other Evaluations :
Given the frequent association of MIS-C with cardiac involvement, many centers are performing baseline cardiac testing including, but not limited to:
- Echocardiogram
- Electrocardiogram
- Chest radiograph, EKG.
- Cardiac enzyme or troponin testing (per the center’s testing standards); and B-type natriuretic peptide (BNP) or NT-proBNP.
- Triglycerides, Creatine kinase, Amylase, Blood and Urine culture, D-dimer, Prothrombin time/Partial Thromboplastin time (PT/PTT), INR, Comprehensive metabolic panel, and Fibrinogen, if not already conducted.
Other testing to evaluate multisystem involvement should be directed by patient signs or symptoms. Additionally, testing to evaluate for other potential diagnoses should be directed by patient signs or symptoms.
Treatment of MIS-C :
There are currently no published guidelines or CDC recommendations regarding treatment for MIS-C and no studies comparing efficacy of various treatment options. Most children with MIS-C need to be treated in a hospital, and some will need treatment in a pediatric intensive care unit. Treatment usually involves different types of therapies that target the immune system and reduce inflammation.
Depending on child's symptoms and condition, he/she may receive anti-inflammatory drugs and other medications to reduce inflammation in the affected vital organs, such as the heart, lungs or kidneys, and protect them from permanent damage. Treatments have consisted primarily of supportive care and directed care against the underlying inflammatory process. Supportive measures have included:
- Fluid resuscitation;
- Inotropic support;
- Respiratory support; and
- In rare cases, extracorporeal membranous oxygenation (ECMO).
- Anti-inflammatory measures have included the frequent use of Intravenous Immunoglobulin (1 to 2 grams/kg), Steroids (ranging from 2 to 30 mg/kg/day of methylprednisolone depending on severity of illness) and Biologics (eg, anakinra, 2 to 10 mg/kg/day, subcutaneously or intravenously, divided every 6 to 12 hours).
- Hematology consultation for assessment of clotting risk and treatment/prophylaxis is recommended (eg, low-dose aspirin, at a minimum, for patients with Kawasaki disease-like syndrome or enoxaparin in patients with thrombosis).
- The use of other anti-inflammatory medications and the use of anti-coagulation treatments have been variable. Aspirin has commonly been used due to the concern for coronary involvement, and antibiotics are routinely used to treat potential sepsis while awaiting bacterial cultures.
MIS-C is not contagious, but there's a chance that child could have an active infection with the COVID-19 virus or another type of contagious infection. So the hospital will use infection control measures while caring for child.
Prevention of MIS-C :
The best way to prevent MIS-C is to take action to avoid exposure to the COVID-19 virus and teach child how to do the same. Follow the guidelines of the U.S. Centers for Disease Control and Prevention:
- Keep hands clean: Wash hands often with soap and water for at least 20 seconds. If soap and water aren't available, use a hand sanitizer that contains at least 60% alcohol.
- Avoid people who are sic: In particular, avoid people who are coughing, sneezing or showing other signs and symptoms that indicate they might be sick and contagious.
- Practice social distancing: This means that person should stay at least 6 feet (2 meters) from other people when outside of home.
- Wear cloth face masks in public settings: When it's difficult to practice social distancing, should wear face masks that cover the nose and mouth (age 2 years or older).
- Clean and disinfect high-touch surfaces every day: This includes areas of home such as doorknobs, light switches, remotes, handles, countertops, tables, chairs, desks, keyboards, faucets, sinks and toilets.
- Wash clothing and other items as needed: Follow manufacturers' instructions, using the warmest appropriate water setting on washing machine. Remember to include washable plush toys.
CDC is still learning about MIS-C and how it affects children, so we don’t know why some children have gotten sick with MIS-C and others have not. We also do not know if children with certain health conditions are more likely to get MIS-C. These are among the many questions CDC is working to try to understand. The best way to prevent MIS-C is to avoid being exposed to infectious virus. However, as a reminder, CDC always recommends everyday preventive actions to help prevent the spread of MIS-C.