Parkinson’s disease (PD) is a chronic progressive neurological disorder that affects predominately dopamine-producing neurons in a specific area of the brain (substantia nigra) characterized by shaking, stiffness and difficulty with walking, balance and coordination that affects movement. It develops gradually, sometimes starting with a barely noticeable tremor in just one hand. But while a tremor may be the most well-known sign of Parkinson's disease, the disorder also commonly causes stiffness or slowing of movement.
In the early stages of Parkinson's disease, face of the patient may show little or no expression, or arms may not swing when walk. Patient’s speech may become soft or slurred. Parkinson's disease symptoms worsen as patient condition progresses over time. Although Parkinson's disease can't be cured, medications may markedly improve your symptoms. In occasional cases, your doctor may suggest surgery to regulate certain regions of your brain and improve your symptoms.
More than 10 million people worldwide are living with Parkinson’s disease. Incidence of Parkinson’s disease increases with age, but an estimated four percent of people with Parkinson’s disease are diagnosed before age 50. Men are 1.5 times more likely to have Parkinson's disease than women.
Nearly one million will be living with Parkinson's disease in the U.S. by 2020, which is more than the combined number of people diagnosed with multiple sclerosis, muscular dystrophy and Lou Gehrig's disease (Amyotrophic Lateral Sclerosis). Approximately 60,000 Americans are diagnosed with Parkinson’s disease each year. The National Institutes of Health (NIH) note that, in the United States, around 50,000 people receive a diagnosis of PD each year, and around half a million people are living with the condition.The prevalence of PD in the U.K. is about one in 500 people, with a total of about 127,000 people living with the disease.
There is no homogeneous and large epidemiological data on Parkinson’s disease from India. Reported a crude prevalence rate of 14.1 per 100,000 amongst a population of 63,645 from rural Kashmir in the northern part of India. The prevalence rate over the age of 60 years was 247/100,000. A low prevalence rate of 27/100,000 was reported from Bangalore, in the southern part of India, and 16.1/100,000 from rural Bengal, in the eastern part of India. Reported a high crude prevalence rate of 328.3/100,000 among a population of 14,010 living in colonies in Mumbai, Western India.
Causes of Parkinson's disease
Parkinson's disease affects about one million people in the United States and ten million worldwide. The main finding in brains of people with Parkinson's is loss of dopaminergic neurons in the area of the brain known as the substantia nigra. In Parkinson's, certain nerve cells (neurons) in the brain gradually break down or die. Many of the symptoms are due to a loss of neurons that produce a chemical messenger in the brain called dopamine. When dopamine levels decrease, it causes abnormal brain activity, leading to signs of Parkinson's disease. The cause of PD is unknown, but several factors appear to play a role, including:
- Genetic Factor : Genetics cause about 10 to 15 percent of all Parkinson's patients. Researchers have identified specific genetic mutations that can cause Parkinson's, but these are uncommon except in rare cases with many family members affected by PD. However, certain gene variations appear to increase the risk of Parkinson's disease but with a relatively small risk of PD for each of these genetic markers.
- Environmental Triggers : Exposure to certain toxins or environmental factors may increase the risk of later PD, but the risk is relatively small. Some environmental exposures may lower the risk of PD, while others may increase it. Environmental risk factors associated with PD include head injury, area of residence, exposure to pesticides and more.
- Parkinson's is caused by a combination of genes, environmental and lifestyle influences. The interaction of all three components determines if someone will develop Parkinson's.
- Researchers have also noted that many changes occur in the brains of people with PD, although it's not clear why these changes occur. These changes include the presence of Lewy bodies [Clumps of specific substances within brain cells are microscopic markers of PD called Lewy bodies. Researchers believe these Lewy bodies hold an important clue to the cause of PD.] and or Alpha-synuclein is found within Lewy bodies [the natural and widespread protein called alpha-synuclein (A-synuclein). It's found in all Lewy bodies in a clumped form that cells can't break down. This is currently an important focus among Parkinson's disease researchers.].
While there’s no known cause, Physician has identified groups of people who are more likely to develop the condition. These include:- Sex: Men are one and a half times more likely to get Parkinson’s than women.
- Race: Whites are more likely to get Parkinson’s disease than African Americans or Asians.
- Age: Parkinson’s disease usually appears between the ages of 50 and 60. It only occurs before the age of 40 in 5-10 percent of cases.
- Family history: People who have close family members with Parkinson’s disease are more likely to develop Parkinson’s disease, too.
- Toxins: Exposure to certain toxins may increase the risk of Parkinson’s disease.
- Head injury: People who experience head injuries may be more likely to develop Parkinson’s disease.
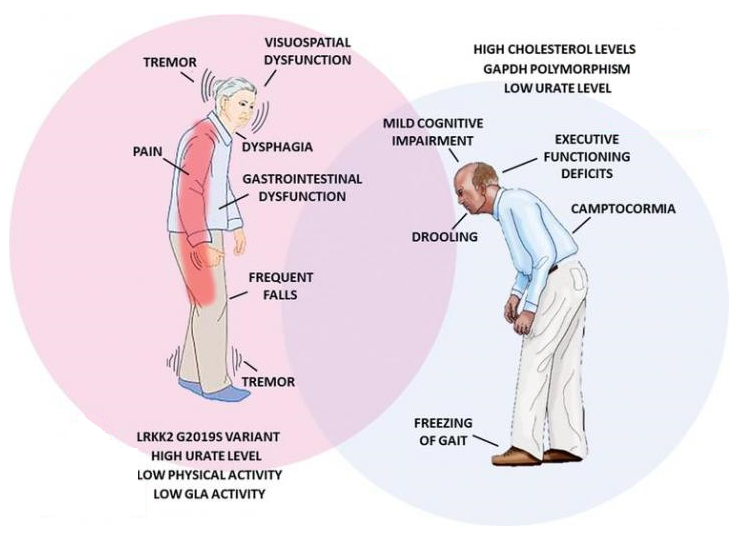
Sign & Symptoms of Parkinson’s Disease
Parkinson's disease symptoms and signs may vary from person to person. Early signs may be mild and may go unnoticed. Symptoms often begin on one side of the body and usually remain worse on that side, even after symptoms begin to affect both sides.
The earliest signs include decreased ability to smell (anosmia), constipation, small & cramped handwriting, voice changes, stooped posture, blank facial expression, a tendency to get stuck when walking, muffled with low-volume speech, decreased blinking and swallowing, tendency to fall backward and reduced arm swinging when walking.
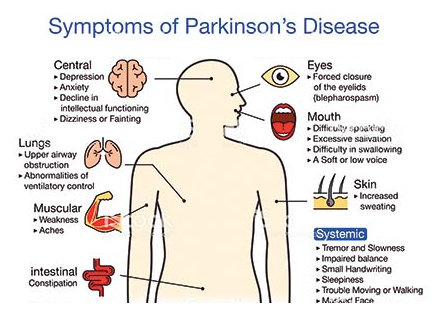
Parkinson's signs and symptoms may include :
- Tremor : A tremor, or shaking, usually begins in a limb, often patient’s hand or fingers. Patient may notice a back-and-forth rubbing of the thumb and forefinger, known as a pill-rolling tremor. One characteristic of Parkinson's disease is a tremor of the hand when it is relaxed (at rest).
- Slowed movement (bradykinesia) : Parkinson's disease may reduce the ability to move and slow the movement, making simple tasks difficult and time-consuming. Steps of the patient may become shorter when walk, or may find it difficult to get out of a chair. Also, patient may drag his/her feet as he/she try to walk, making it difficult to move.
- Rigid muscles : Muscle stiffness may occur in any part of the body. The stiff muscles can limit range of motion and cause pain.
- Impaired Posture and Balance : Posture of the patient may become stooped, or he/she may have balance problems as a result of Parkinson's disease.
- Loss of automatic movements : In Parkinson's disease, Patient may have a decreased ability to perform unconscious movements, including blinking, smiling or swinging your arms when walk.
- Speech changes : Patient may have speech problems as a result of Parkinson's disease. He/She may speak softly, quickly, slur or hesitate before talking. Patient’s speech may be more of a monotone rather than with the usual inflections.
- Writing changes : It may become hard to write, and his/her writing may appear small.
If the Parkinson's disease is not discovered on the early stage then the sign & symptoms become more serious, symptoms may include flaky white or yellow scales on oily parts of the skin (seborrheic dermatitis), increased risk of melanoma, sleep disturbances including vivid dreams, talking, and movement during sleep, depression, anxiety, hallucinations, psychosis, problems with attention and memory, difficulty with visual-spatial relationships etc.
Diagnosis of Parkinson’s Disease
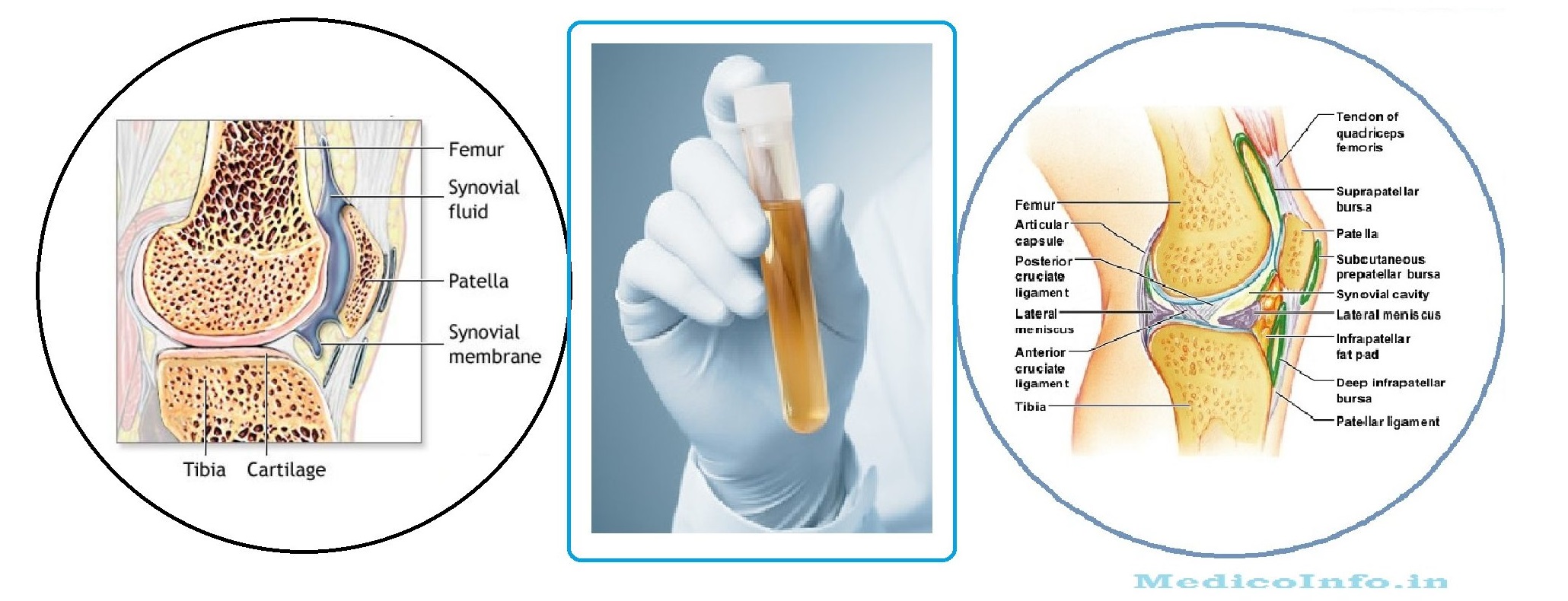
There’s no specific test for diagnosing Parkinson’s. A number of disorders can cause symptoms similar to those of Parkinson's disease. Diagnosis of Parkinson’s disease is made based on the patient’s health history, a physical and neurological exam, as well as a review of signs and symptoms. Physician may order tests, such as blood tests, imaging test to rule out other conditions that may be causing symptoms of Parkinson’s disease.
Imaging tests : Such as MRI, CAT Scan, Ultrasound of the brain, SPECT and PET scans - may also be used to help rule out other disorders. A Dopamine transporter (DAT) scan may also be used. Imaging tests aren't particularly helpful for diagnosing Parkinson's disease.
In addition to examination, doctor may give carbidopa-levodopa, a Parkinson's disease medication. Patient must be given a sufficient dose to show the benefit, as low doses for a day or two aren't reliable. Significant improvement with this medication will often confirm diagnosis of Parkinson's disease. Sometimes it takes time to diagnose Parkinson's disease. Doctors may recommend regular follow-up appointments with neurologists trained in movement disorders to evaluate the condition and symptoms over time and diagnose Parkinson's disease.
Complications of Parkinson’s Disease
Parkinson's disease is often accompanied by these additional problems, which may be treatable:
- Thinking difficulties : Patient may experience cognitive problems (dementia) and thinking difficulties, which usually occur in the later stages of Parkinson's disease. Such cognitive problems aren't very responsive to medications.
- Depression and emotional changes : People with Parkinson's disease may experience depression. Receiving treatment for depression can make it easier to handle the other challenges of Parkinson's disease. Patient may also experience other emotional changes, such as fear, anxiety or loss of motivation. Doctors may give medications to treat these symptoms.
- Swallowing problems : Patient may develop difficulties with swallowing as condition progresses. Saliva may accumulate in the mouth due to slowed swallowing, leading to drooling.
- Sleep problems and sleep disorders : People with Parkinson's disease often have sleep problems, including waking up frequently throughout the night, waking up early or falling asleep during the day. He/She may also experience rapid eye movement sleep behavior disorder, which involves acting out his/her dreams. Medications may help to recovery the sleep problems.
- Bladder problems : Parkinson's disease may cause bladder problems, including being unable to control urine or having difficulty urinating.
- Constipation : Many people with Parkinson's disease develop constipation, mainly due to a slower digestive tract.
- Blood pressure changes : Patient may feel dizzy or lightheaded when stand due to a sudden drop in blood pressure (orthostatic hypotension).
- Smell dysfunction : Patient may experience problems with sense of smell. He/She may have difficulty identifying certain odors or the difference between odors.
- Fatigue : Many people with Parkinson's disease lose energy and experience fatigue, and the cause isn't always known.
- Pain : Many people with Parkinson's disease experience pain, either in specific areas of their bodies or throughout their bodies.
- Sexual dysfunction : Some people with Parkinson's disease notice a decrease in sexual desire or performance.
Treatment of Parkinson’s disease
Parkinson’s disease can't be cured, but medications can help control the symptoms, often dramatically. In some later cases, surgery may be advised. Doctor may also recommend lifestyle changes, especially ongoing aerobic exercise. In some cases, physical therapy that focuses on balance and stretching also is important. A speech-language pathologist may help improve speech problems.
A. Medications :
Medications may help to manage problems with walking, movement and tremor. These medications increase or substitute for dopamine, a specific signaling chemical (neurotransmitter) in the brain. People with PD have low brain dopamine concentrations.
However, dopamine can't be given directly, as it can't enter in the brain. Patient may have significant improvement of his/her symptoms after beginning Parkinson's disease treatment. Over time, however, the benefits of drugs frequently diminish or become less consistent, although symptoms usually can continue to be fairly well-controlled. Medications may prescribe include:
- Carbidopa-levodopa. Levodopa : Carbidopa-levodopa. Levodopa, the most effective Parkinson's disease medication, is a natural chemical that passes into the brain and is converted to dopamine. Levodopa is combined with carbidopa (Rytary, Sinemet), which protects levodopa from premature conversion to dopamine outside the brain, which prevents or lessens side effects such as nausea. Side effects may include nausea or lightheadedness (orthostatic hypotension). After years, as the disease progresses, the benefit from levodopa may become less stable, with a tendency to wax and wane ("wearing off"). Also, patient may experience involuntary movements (dyskinesia) after taking higher doses of levodopa. Doctor may lessen the dose of the medicine or adjust the times of the doses to control these effects.
- Carbidopa-levodopa infusion : The U.S. Food and Drug administration approved a drug called Duopa in 2015. This medication is made up of carbidopa and levodopa. However, it's administered through a feeding tube that delivers the medication in a gel form directly to the small intestine. Duopa is for patients with more advanced Parkinson's who still respond to carbidopa-levodopa, but who have a lot of fluctuations in their response. Because Duopa is continually infused, blood levels of the two drugs remain constant. Placement of the tube requires a small surgical procedure. Risks associated with having the tube include the tube falling out or infections at the infusion site.
- Dopamine agonists : Unlike levodopa, dopamine agonists don't change into dopamine. Instead, they mimic dopamine effects in the patient’s brain. They aren't as effective as levodopa in treating the symptoms. However, they last longer and may be used with levodopa to smooth the sometimes off-and-on effect of levodopa. Dopamine agonists include pramipexole (Mirapex), ropinirole (Requip) and rotigotine (given as a patch, Neupro). A short-acting injectable dopamine agonist, apomorphine (Apokyn), is used for quick relief. Some of the side effects of dopamine agonists are similar to the side effects of carbidopa-levodopa, but also include hallucinations, sleepiness and compulsive behaviors such as hypersexuality, gambling and eating.
- MAO-B inhibitors : These medications include selegiline (Eldepryl, Zelapar) and rasagiline (Azilect). They help prevent the breakdown of brain dopamine by inhibiting the brain enzyme monoamine oxidase B (MAO-B). This enzyme metabolizes brain dopamine. Side effects may include nausea or insomnia. When added to carbidopa-levodopa, these medications increase the risk of hallucinations. These medications are not often used in combination with most antidepressants or certain narcotics due to potentially serious but rare reactions. Check with doctor before taking any additional medications with a MAO-B inhibitor.
- Catechol-O-methyltransferase (COMT) inhibitors : Entacapone (Comtan) is the primary medication from this class. This medication mildly prolongs the effect of levodopa therapy by blocking an enzyme that breaks down dopamine. Side effects, including an increased risk of involuntary movements (dyskinesias), mainly result from an enhanced levodopa effect. Other side effects include diarrhea or other enhanced levodopa side effects. Tolcapone (Tasmar) is another COMT inhibitor that is rarely prescribed due to a risk of serious liver damage and liver failure.
- Anticholinergics : These medications were used for many years to help control the tremor associated with Parkinson's disease. Several anticholinergic medications are available, including benztropine (Cogentin) or trihexyphenidyl. However, their modest benefits are often offset by side effects such as impaired memory, confusion, hallucinations, constipation, dry mouth and impaired urination.
- Amantadine : Doctors may prescribe amantadine alone to provide short-term relief of symptoms of mild, early-stage Parkinson's disease. It may also be given with carbidopa-levodopa therapy during the later stages of Parkinson's disease to control involuntary movements (dyskinesias) induced by carbidopa-levodopa. Side effects may include a purple mottling of the skin, ankle swelling or hallucinations.
B. Surgical procedures
Deep Brain Stimulation (DBS) : In deep brain stimulation (DBS), surgeons implant electrodes into a specific part of the brain. The electrodes are connected to a generator implanted in the patient chest near the collarbone that sends electrical pulses to the brain and may reduce PD symptoms. Doctor may adjust the settings as necessary to treat his/her condition. Surgery involves risks, including infections, stroke or brain hemorrhage. Some people experience problems with the DBS system or have complications due to stimulation, and doctor may need to adjust or replace some parts of the system.
Deep brain stimulation is most often offered to people with advanced Parkinson's disease who have unstable medication (levodopa) responses. DBS can stabilize medication fluctuations, reduce or halt involuntary movements (dyskinesias), reduce tremor, reduce rigidity, and improve slowing of movement.
DBS is effective in controlling erratic and fluctuating responses to levodopa or for controlling dyskinesias that don't improve with medication adjustments. However, DBS isn't helpful for problems that don't respond to levodopa therapy apart from tremor. A tremor may be controlled by DBS even if the tremor isn't very responsive to levodopa. Although DBS may provide sustained benefit for Parkinson's symptoms, it doesn't keep Parkinson's disease from progressing.
Prevention of Parkinson’s Disease
Because the cause of Parkinson's is unknown, proven ways to prevent the disease also remain a mystery. However, some research has shown that caffeine — which is found in coffee, tea and cola — may reduce the risk of developing Parkinson's disease. Green tea also may reduce the risk of developing PD. Some research has shown that regular aerobic exercise may reduce the risk of Parkinson's disease.
For people diagnosed with Parkinson’s, diet can play an important role in daily life. While it will not treat or prevent progression, a healthy diet may have some significant impacts. Parkinson’s is the result of decreased dopamine levels in the brain. Patient may be able to increase levels of the hormone naturally with food. Likewise, a healthy diet that focuses on specific nutrients may be able to reduce some symptoms and prevent progression of the disease.
These foods include Antioxidants (prevent oxidative stress and damage to the brain. Antioxidant-rich foods include nuts, berries, and nightshade vegetables.), Fava beans (contain levodopa, the same ingredient used in some Parkinson’s medications.) and Omega-3s (heart- and brain-healthy fats in salmon, oyster, flax seed, and some beans may help protect the brain from damage.) In addition to eating more of these beneficial foods, may want to avoid dairy and saturated fat. These food groups may increase the risk for Parkinson’s or speed up progression.