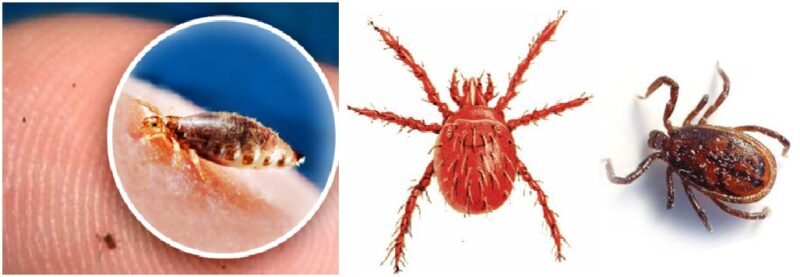
Scrub typhus is a disease caused by a bacteria called Orientia tsutsugamushi (rickettsial bacteria); it’s also known as tsutsugamushi disease or bush typhus . The most common symptoms of scrub typhus include fever, headache, body aches, and sometimes rash and untreated typhus can lead to serious complications and it’s potentially fatal. Scrub typhus is spread to people through bites of infected chiggers (mites), Fleas, lice or ticks transmit. When Fleas, mites, lice, and ticks carrying rickettsial bacteria and bite someone the bacteria transmit into the patient blood stream. Once in the bloodstream, the bacteria continue to reproduce and grow that causes typhus. There are three different types of typhus: Epidemic (louse-borne) typhus, Endemic (murine) typhus and Scrub typhus. These are caused by three different types of typhus, and each type is caused by a different type of bacterium and transmitted by a different type of arthropod. Typhus is not transmitted from person to person like a cold or the flu. 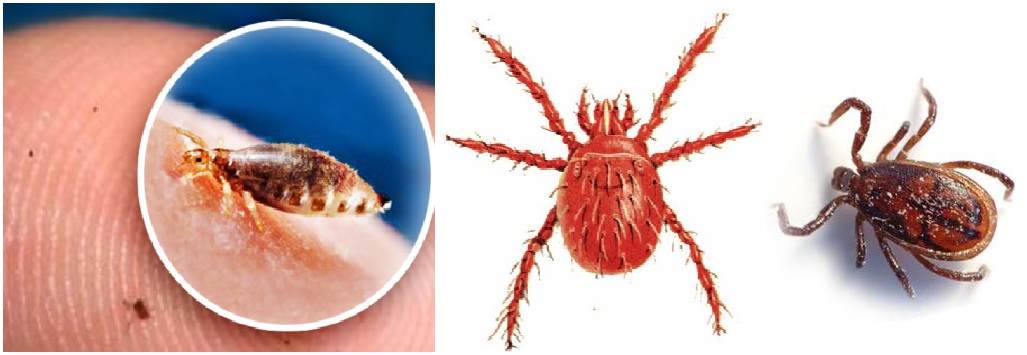 Most cases of scrub typhus occur in rural areas of developing countries or in regions of poverty, poor sanitation and close human contact. Scrub typhus is generally occur in the rural region of Southeast Asia, Indonesia, China, Japan, India, and northern Australia. Anyone living in or traveling to areas where scrub typhus is found could get infected. The highest rates are seen in the older adults and those who are malnourished. Children usually recover from typhus. People with underlying diseases such as diabetes mellitus, alcoholism or chronic renal disorders also have a higher risk of mortality. Mortality rate for Scrub typhus that goes untreated can range upto 30% worldwide.
Most cases of scrub typhus occur in rural areas of developing countries or in regions of poverty, poor sanitation and close human contact. Scrub typhus is generally occur in the rural region of Southeast Asia, Indonesia, China, Japan, India, and northern Australia. Anyone living in or traveling to areas where scrub typhus is found could get infected. The highest rates are seen in the older adults and those who are malnourished. Children usually recover from typhus. People with underlying diseases such as diabetes mellitus, alcoholism or chronic renal disorders also have a higher risk of mortality. Mortality rate for Scrub typhus that goes untreated can range upto 30% worldwide.
Signs and Symptoms
Symptoms of scrub typhus usually begin within 10 days of being bitten. Signs and symptoms may include:
- Fever and chills
- Headache
- Body aches and muscle pain
- A dark, scab-like region at the site of the chigger bite (also known as eschar)
- Mental changes, ranging from confusion to coma
- Enlarged lymph nodes
- Rash
People with severe illness may develop organ failure and bleeding, which can be fatal and also untreated typhus can lead to serious complications and it’s potentially fatal.
Diagnosis and Examination
Diagnosis of Scrub typhus is very difficult because symptoms are common to other infectious diseases like Dengue (breakbone fever), Malaria (disease spread by mosquitos) and brucellosis. Just because symptoms of scrub typhus are similar to symptoms of many other diseases. So immediate physician consultation is required if the patient have fever, headache, body aches and any type rash. If the patient have recently traveled, tell his/her physician where and when traveled then the physician may order blood tests to look for scrub typhus or other diseases and he/she may start treatment before results are available. 
Diagnostic tests for the presence of typhus include:
- Skin biopsy : a specimen of the skin from the rash will be tested in a laboratory.
- Enzyme-Linked Immunosorbent Assay (ELISA) : Detection of antibodies against infectious agents use pooled human sera as reference material to establish cut-off values and to routinely confirm test integrity. The 56-kDa protein (located on the outer membrane of O. Tsutsugamushi) is highly reactive with patient sera and therefore preferred for use in the diagnosis of scrub typhus.
- Rapid Lateral Flow Assay : Consists of a single strip (IgG, IgM), where the Kp r56 protein was conjugated to gold particles as the indicator system.
- Western Blot : Assay r56 from the Karp, Kato, and Gilliam strains of O. Tsutsugamushi (KpKtGm r56),using electrophoresis. Results are interpreted as positive or negative.
- Immunochromatographic Assay : A rapid diagnostic test in which serum is applied to the reagent pad of the ICT strip. The results is recorded as positive, equivocal, or negative for the presence of the control and the IgM or total antibody lines.
- Indirect Fluorescent Assay (IFA) : It has been considered as the gold standard for serologic detection of scrub typhus antibodies and is also currently the reference standard.
- Indirect Immunoperoxidase Assay : This test has the advantage in that any rickettsial strain can be used as the antigen, either IgG or IgM antibodies can be titrated individually.
- PCR Amplification of Orientia Genes : It’s may be the most sensitive diagnostic test, can detect the organism as early as 1-3 days of the fever phase. Samples from eschars or blood are used for this assay. Since O. tsutsugamushi is an intracellular organism, thus whole blood or the buffy coat is considered to be the preferred samples for PCR tests.
- Isolation or Inoculation of Agent : tsutsugamushi can be isolated and cultured from a patient’s blood by inoculating it intraperitoneally, into white mice under biosafety level-3 facilities.
Treatment & Complication
Early treatment with antibiotics is very effective and relapses aren’t common if the patient take the full course of antibiotics. Delayed treatment and misdiagnosis can lead to a more severe. Immediate treatment required for suspected case where the patient have fever, headache, body aches, and any type rash….
- Scrub typhus should be treated with the antibiotic doxycycline. Doxycycline can be used in persons of any age.
- Antibiotics are most effective if given soon after symptoms begin.
- People who are treated early with doxycycline usually recover quickly.
- Other antibiotics most commonly used to treat typhus include:
- Chloramphenicol : An option for pregnant or breastfeeding.
- Ciprofloxacin : used for adults who are unable to take Doxycycline.
Some common complications of Scrub typhus include Hepatitis, Gastrointestinal hemorrhage and hypovolemia etc.
Prevention
The easiest way to prevent typhus is by avoiding the pests that spread it.
Suggestions for prevention include:
- maintaining adequate personal hygiene.
- controlling the rodent population.
- avoiding travel to regions where typhus exposure has occurred, or to countries that are high risk due to lack of sanitation
- chemoprophylaxis with doxycycline (used as a preventive only in those at high risk, such as those on humanitarian campaigns in areas with extreme poverty and little or no sanitation)
- Use tick, mite, and insect repellant. Perform routine examinations for ticks and wear protective clothing if you’re traveling near an area where there have been typhus outbreaks.
- No vaccine is available to prevent scrub typhus.
- Reduce your risk of getting scrub typhus by avoiding contact with infected chiggers.
- When traveling to areas where scrub typhus is common, avoid areas with lots of vegetation and brush where chiggers may be found.
- If you have a baby or child then dress your child in clothing that covers arms and legs, or cover crib, stroller, and baby carrier with mosquito netting etc.