Alzheimer’s Disease : Sign & Symptoms, Causes, Stages, Risk factors, Diagnosis, Complication, Treatment and Prevention
Alzheimer's disease (AD) is a chronic irreversible progressive neurodegenerative disease characterized by dementia, destruction of memory and other important mental functions like confusion, difficulty remembering and impulsive or unpredictable behavior that usually starts slowly and gets worse over time. It's commonly known as Alzheimer's. At starting phase, people with Alzheimer's disease may notice mild confusion and difficulty remembering because of the brain cells degenerate and die, causing a steady decline in memory and mental function. Afterwards may even forget important people in their lives and undergo dramatic personality changes.

It is named after Dr. Alois Alzheimer, who first described the condition in 1906. Alzheimer’s disease (AD) is the most common disease of aging. One of the main features of the Alzheimer's disease is the presence of plaques and tangles in the brain. Another feature is a loss of connection between the nerve cells, or neurons in the brain.
There’s no cure for Alzheimer’s disease, but there are treatments that can slow the progression of the disease and may improve quality of life. Initially medications and management may temporarily improve symptoms. But because there's no cure of the disease, it's important to seek supportive services and tap into support network as early as possible.
According to the Alzheimer’s Association, early onset Alzheimer’s disease affects around 200,000 U.S. adults under the age of 65 years. Many people with this condition are in their 40s or 50s. According to the National Institute on Aging, Alzheimer’s disease is the sixth leading cause of death in the U.S. However, other recent estimates suggest that it may be the third leading cause of death, just behind heart disease and cancer.
Sign & Symptoms of Alzheimer’s disease
The most common early symptom of Alzheimer's is difficulty remembering newly learned information because Alzheimer's changes typically begin in the part of the brain that affects learning. As Alzheimer's advances through the brain it leads to increasingly severe symptoms, including disorientation, mood & behavior changes; deepening confusion about events, time and place; unfounded suspicions about family, friends and professional caregivers; more serious memory loss and behavior changes; and difficulty speaking, swallowing and walking. A family member or friend may be more likely to notice how the symptoms worsen. Brain changes associated with Alzheimer's disease lead to growing trouble with:
A. Memory
Everyone has occasional memory lapses, but the memory loss associated with Alzheimer's disease persists and worsens, affecting the ability to function at work or at home. People with Alzheimer's may:
-
- Repeat statements and questions over and over.
- Forget conversations, appointments or events, and not remember them later.
- Routinely misplace possessions, often putting them in illogical locations.
- Get lost in familiar places.
- Eventually forget the names of family members and everyday objects.
- Have trouble finding the right words to identify objects, express thoughts or take part in conversations.
B. Thinking and reasoning :
Alzheimer's disease causes difficulty concentrating and thinking, especially about abstract concepts such as numbers.
-
- Multitasking is especially difficult, and it may be challenging to manage finances, balance checkbooks and pay bills on time. Eventually, a person with Alzheimer's may be unable to recognize and deal with numbers.
- Alzheimer’s personnel can lose track of dates, seasons and the passage of time. They may have trouble understanding something if it is not happening immediately. Sometimes they may forget where they are or how they got there.
C. Making judgments and decisions :
Alzheimer's causes a decline in the ability to make reasonable decisions and judgments in everyday situations. It may be more difficult to respond effectively to everyday problems, such as food burning on the stove or unexpected driving situations.
-
- For some people, having vision problems is a sign of Alzheimer's. This may lead to difficulty with balance or trouble reading. They may also have problems judging distance and determining color or contrast, causing issues with driving.
- Once-routine activities that require sequential steps, such as planning and cooking a meal or playing a favorite game, become a struggle as the disease progresses. Eventually, people with advanced Alzheimer's often forget how to perform basic tasks such as dressing and bathing.
- A person may have difficulty with their balance, trip over, or spill things more often, or they may have difficulty orienting clothing to their body when getting dressed.
- A person may develop difficulties with thinking of common words, or they may make more speech, spelling, or writing errors.
D. Changes in personality and behavior :
Brain changes that occur in Alzheimer's disease can affect moods and behaviors. Problems may include the following:
-
- Depression
- Apathy
- Compulsive, obsessive, or socially inappropriate behavior
- Mood swings, becoming upset, angry, or worried more often than before.
- Distrust in others & lose of empathy.
- Irritability and aggressiveness
- Changes in sleeping habits
- Wandering
- Loss of inhibitions
- Delusions, such as believing something has been stolen.
- A loss of interest in or motivation for activities they usually enjoy.
A person may develop difficulties with thinking of common words, or they may make more speech, spelling, or writing errors at the advance stage. Many important skills are not lost until very late in the disease. These include the ability to read, dance and sing, enjoy old music, engage in crafts and hobbies, tell stories, and reminisce.
Stages of Alzheimer’s Disease
Alzheimer’s disease can range from mild to severe as per the severity of sign & symptoms. The scale ranges from a state of mild impairment, through to moderate impairment, before eventually reaching severe cognitive decline.
Mild Alzheimer’s disease :
People with mild Alzheimer’s disease develop memory problems and cognitive difficulties that may include the following:
-
- Taking longer than usual to perform daily tasks.
- Difficulty handling money or paying the bills.
- While performing fine motor tasks such as writing, drawing, or dressing, certain movement coordination and planning difficulties may be present.
- Wandering and getting lost.
- Experiencing personality and behavior changes, such as getting upset or angry more easily, hiding things, or pacing.
- Difficulties with language. Language problems are mainly characterized by a shrinking vocabulary and decreased word fluency, leading to a general impoverishment of oral and written language
Moderate Alzheimer’s disease :
In moderate Alzheimer’s disease, the parts of the brain responsible for language, senses, reasoning, and consciousness are damaged. This can lead to the following symptoms:
-
- Greater memory loss and confusion.
- Speech difficulties become evident (inability to recall vocabulary, which leads paraphasias)
- Reading and writing skills are progressively lost.
- Difficulty recognizing friends or family.
- An inability to learn new things.
- Difficulty performing tasks with several stages, such as getting dressed
- Difficulty coping with new situations
- Impulsive behavior
- Hallucinations, delusions, or paranoia.
Severe Alzheimer’s disease :
In severe Alzheimer’s disease, plaques and tangles are present throughout the brain, causing the brain tissue to shrink substantially. This can lead to:
-
- An inability to communicate. Language is reduced to simple phrases or even single words, eventually leading to complete loss of speech.
- Extreme apathy, exhaustion and aggressiveness can still be present.
- Muscle mass and mobility deteriorates.
- Dependency on others for care.
- Being unable to leave bed all or most of the time.
Causes of Alzheimer’s Disease
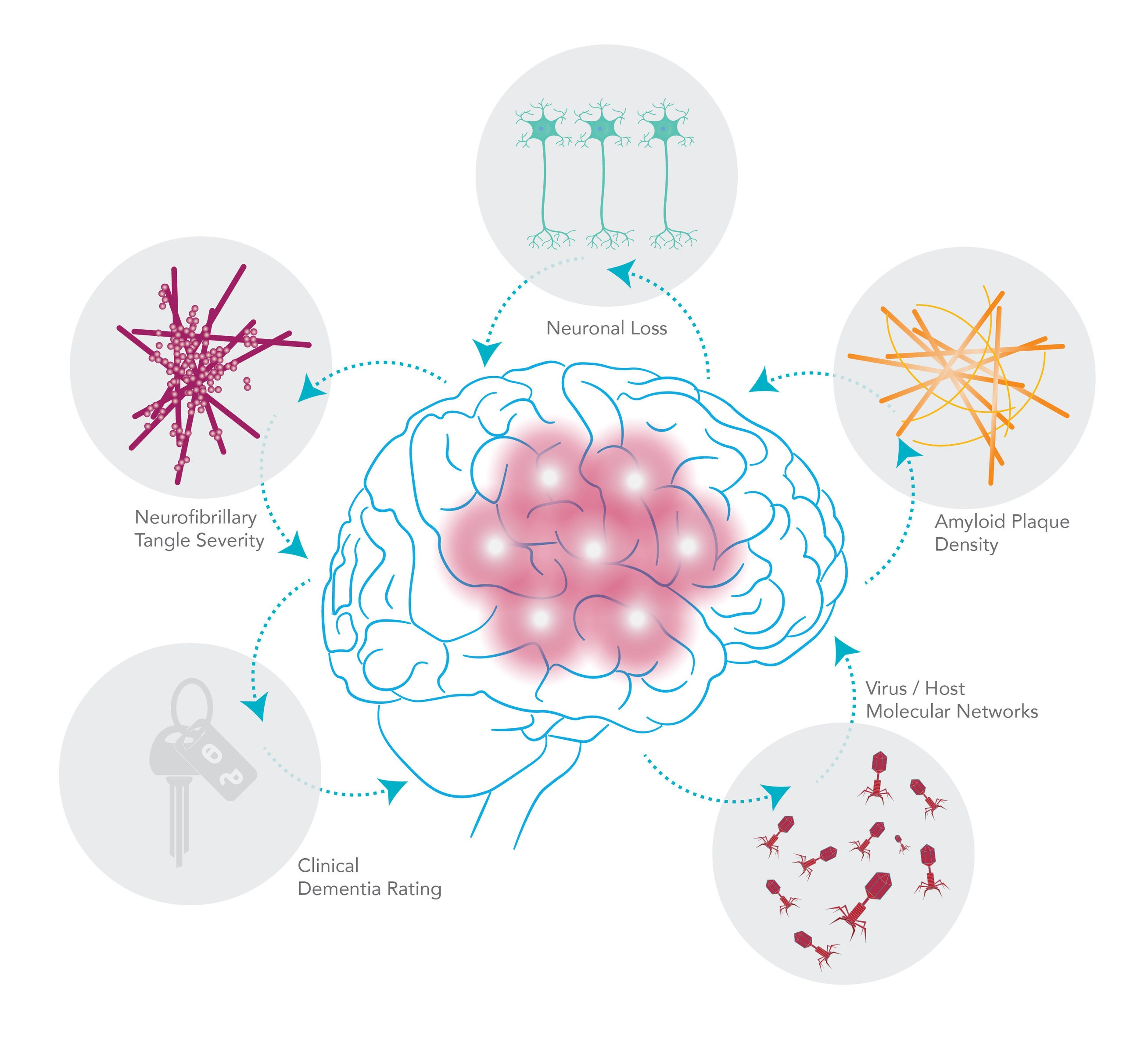
In 1906, Dr. Alzheimer noticed changes in the brain tissue of a woman who had died of an unusual mental illness. Her symptoms included memory loss, language problems and unpredictable behavior. After she died, he examined her brain and found many abnormal clumps (amyloid plaques) and tangled bundles of fibers (neurofibrillary or tau, tangles). These plaques and tangles in the brain are still considered some of the main features of Alzheimer’s disease. Another feature is the loss of connections between nerve cells (neurons) in the brain. Neurons transmit messages between different parts of the brain, and from the brain to muscles and organs in the body.
Though autopsy studies show that most people develop some plaques and tangles as they age, those with Alzheimer’s tend to develop far more and in a predictable pattern, beginning in the areas important for memory before spreading to other regions. Scientists do not know exactly what role plaques and tangles play in Alzheimer's disease. Most experts believe they somehow play a critical role in blocking communication among nerve cells and disrupting processes that cells need to survive. It's the destruction and death of nerve cells that causes memory failure, personality changes, problems carrying out daily activities and other symptoms of Alzheimer's disease.
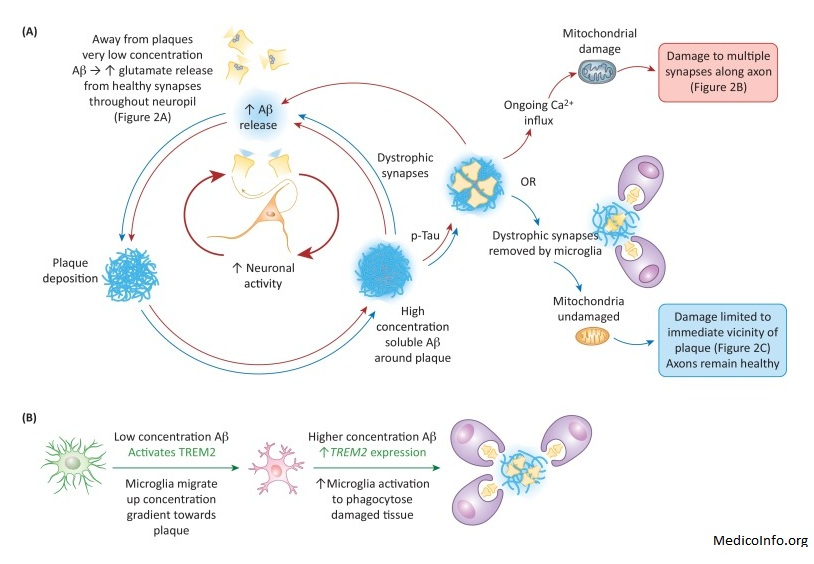 Scientists continue to unravel the complex brain changes involved in the onset and progression of Alzheimer’s disease. It seems likely that changes in the brain may begin a decade or more before memory and other cognitive problems appear. During this preclinical stage of Alzheimer’s disease, people seem to be symptom-free, but toxic changes are taking place in the brain. Abnormal deposits of proteins form amyloid plaques and tau tangles throughout the brain. Once-healthy neurons stop functioning, lose connections with other neurons, and die. Many other complex brain changes are thought to play a role in Alzheimer’s, too.
Scientists continue to unravel the complex brain changes involved in the onset and progression of Alzheimer’s disease. It seems likely that changes in the brain may begin a decade or more before memory and other cognitive problems appear. During this preclinical stage of Alzheimer’s disease, people seem to be symptom-free, but toxic changes are taking place in the brain. Abnormal deposits of proteins form amyloid plaques and tau tangles throughout the brain. Once-healthy neurons stop functioning, lose connections with other neurons, and die. Many other complex brain changes are thought to play a role in Alzheimer’s, too.
The damage initially appears to take place in the hippocampus and the entorhinal cortex; parts of the brain essential in forming memories. As more neurons die, additional parts of the brain are affected and begin to shrink. By the final stage of Alzheimer’s, damage is widespread, and brain tissue has shrunk significantly.
Risk factors of Alzheimer’s disease
Researchers do not fully understand the actual cause of Alzheimer’s disease and why complex brain changes involved in the onset and progression of Alzheimer’s disease. They suspect, several factors may be involved for Alzheimer’s disease as like –
- Age : Advancing age is a primary risk factor for the disease and incidence rates are not equal for all ages. Alzheimer's is not a part of normal aging, but the risk increases greatly after reach age 65 years. Every five years after the age of 65, the risk of acquiring the disease approximately doubles. One of the great mysteries of Alzheimer’s disease is why it largely strikes older adults.
- Sex : Women seem to be more likely than are men to develop Alzheimer's disease, in part because they live longer.
- Genetic factor : Researchers have not found a specific gene that directly causes late-onset Alzheimer’s. However, having one form of the apolipoprotein E (APOE) gene does increase a person’s risk. This gene has several forms. One of them, APOE ε4, increases a person’s risk of developing the disease and is also associated with an earlier age of disease onset. However, carrying the APOE ε4 form of the gene does not mean that a person will definitely develop Alzheimer’s disease, and some people with no APOE ε4 may also develop the disease.
Also, scientists have identified a number of regions of interest in the genome (an organism’s complete set of DNA) that may increase or decrease a person’s risk for late-onset Alzheimer’s to varying degrees.
Early-onset Alzheimer’s disease occurs between a person’s 30s and mid-60s and represents less than 10 percent of all people with Alzheimer’s. Some cases are caused by an inherited change in one of three genes. For others, research shows that other genetic components are involved.
Most people with Down syndrome develop Alzheimer’s. This may be because people with Down syndrome have an extra copy of chromosome 21, which contains the gene that generates harmful amyloid and significantly increases the risk of Alzheimer's disease. - Lifestyle : There's no lifestyle factor that's been definitively shown to reduce risk of Alzheimer's disease. However, some evidence suggests that the same factors that put at risk of heart disease also may increase the chance that person will develop Alzheimer's. Examples include:
- Lack of exercise
- Obesity
- Smoking or exposure to secondhand smoke
- Hypertension
- High blood cholesterol
- Poorly controlled Type-2 diabetes
- A diet lacking in fruits and vegetables.
These risk factors are also linked to vascular dementia; a type of dementia caused by damaged blood vessels in the brain. Working with Healthcare team on a plan to control these factors will help to protect heart - and may also help reduce risk of Alzheimer's disease and vascular dementia.
Other factors that increase the risk of Alzheimer’s include severe or repeated traumatic brain injuries and having exposure to some environmental contaminants, such as toxic metals, pesticides, and industrial chemicals.
Diagnosis of Alzheimer’s disease
The early stages of Alzheimer's disease are difficult to diagnose. A definitive diagnosis is usually made once cognitive impairment compromises daily living activities, although the person may still be living independently. The symptoms will progress from mild cognitive problems, such as memory loss through increasing stages of cognitive and non-cognitive disturbances, eliminating any possibility of independent living, especially in the late stages of the disease.
There is no specific single test for Alzheimer’s disease. If a doctor suspects the presence of the condition, they will ask the person about their past information regarding health, medication, diet, past medical problems, ability to carry out daily activities, changes in behavior and personality. Sometimes consult with their family or caregivers about their symptoms, experiences, medical history and changes in behavior and personality
The only definitive way to diagnose someone with Alzheimer’s disease is to examine their brain tissue after death when microscopic examination of the brain reveals the characteristic plaques and tangles. But doctor can examinations the neurological health, mental abilities, diagnose dementia, and rule out other conditions for diagnosis of Alzheimer’s disease.
- Doctor will perform a physical examination for assess overall neurological health by testing the patient’s joints & muscular reflexes, muscle tone and strength, sense of sight and hearing, coordination & balance. Afterwards mental status analyzed to assess patient’s short-term memory, long-term memory, and orientation to place and time.
- Some of the imaging study may ensure accurate diagnosis of Alzheimer’s disease these are as follows :
- Computed Tomography (CT) scan: A CT scan uses x-ray technology to create multiple images of the brain. It helps detect conditions like bleeding in the brain, inflammation, skull fractures, blood clots, strokes, brain tumors, enlarged brain cavities, other signs of brain disease.
- Magnetic Resonance Imaging (MRI): An MRI takes multiple images of the brain using powerful magnets and radio waves. It can helps to detect cysts, tumors, bleeding, swelling, structural abnormalities, infections, inflammatory conditions or/and problems with the blood vessels in the brain.
- Positron Emission Tomography (PET) scan: A PET scan is an imaging test that can provide information on how the brain and its tissues function on a cellular level. It’s used to detect changes in bodily processes that can reveal abnormalities of brain function. These include changes in glucose metabolism, oxygen metabolism, blood flow etc.
During a PET scan, a low-level radioactive tracer is injected into the blood to reveal a particular feature in the brain. Fluorodeoxyglucose (FDG) PET scans show areas of the brain in which nutrients are poorly metabolized, identifying patterns of degeneration, areas of low metabolism. It can help to distinguish between Alzheimer's disease and other types of dementia. Amyloid PET imaging can measure the burden of amyloid deposits in the brain. Tau PET imaging can measures the burden of neurofibrillary tangles in the brain. Amyloid & Tau PET imaging are generally used in the research purpose.
- Some time doctor may suggest for few blood investigations to rule out other potential causes of memory loss and confusion, such as some hereditary genetic analysis (mutations in the amyloid precursor protein, presenilin-1, or presenilin-2 genes and APOEɛ4 genes etc.), thyroid disorders or vitamin & mineral deficiencies. There are few genes such as APP (on chromosome 21), PSEN1 (on chromosome 14), and PSEN2 (on chromosome 1); People with mutations on one or more of these genes tend to develop early-onset Alzheimer’s disease.
- In special circumstances, Cerebrospinal fluid (CSF) analysis may be used to measure abnormal beta-amyloid and tau in the CSF.
Genetic testing generally isn't recommended for a routine Alzheimer's disease evaluation. The exception is people who have a history of early-onset Alzheimer's disease. However, anyone with family history of early Alzheimer's needs to meet with a Genetic counselor to discuss the risks and benefits of genetic testing.
Complications of Alzheimer’s Disease
Alzheimer’s disease has many side effects and complications that can create problems for the patient and their caregivers. It is important for all caregivers to be aware of these conditions to minimize problems. At starting phase, people with Alzheimer's disease may notice mild confusion and difficulty remembering because of the brain cells degenerate and die, causing a steady decline in memory and mental function. Afterwards may even forget important people in their lives and undergo dramatic personality changes. Initially medications and management may temporarily improve symptoms. But because there's no cure of the disease, it's important to seek supportive services and tap into support network as early as possible.
- People who have Alzheimer’s disease may fall, which can cause serious injuries. Many people with the disease have to use a cane or walker, but they may not remember that they need to use them. That is how many serious falls can happen.
- A Urinary Tract Infection (UTI) is another common complication of which caregivers should be aware. They are particularly frequent in the mid to late stages of the disease, as incontinence becomes more of an issue. So, many people who have the disease must use a catheter. These often are needed, but they can bring bacteria into the body and cause a UTI.
- Bedsores occur when a person sits or lies in bed for a prolonged period of time in one position, causing the breakdown of the skin because of prolonged pressure on the area. In the late stages of Alzheimer’s, it is harder to move, so the patient might be lying down or sitting in one place more.
- As Alzheimer’s progresses, the patient might find that they forget to eat or drink, or find that they lose their appetite more often. It might also be harder for them to swallow or eat. This can lead to pneumonia in the later stages of the disease. This can happen because the patient is not able to communicate pain and discomfort to the caregiver.
As Alzheimer's disease progresses to its last stages, brain changes begin to affect physical functions such as swallowing, balance, and bowel and bladder control. These effects can increase vulnerability to additional health problems such as inhaling food or liquid into the lungs (aspiration), pneumonia and other infections, falls, fractures, bedsores and malnutrition or dehydration etc.
Treatment & Prevention of Alzheimer's disease
There’s no cure for Alzheimer’s disease, but there are treatments that can slow the progression of the disease and may improve quality of life. Initially medications and management may temporarily improve symptoms. But because there's no cure of the disease, it's important to seek supportive services and tap into support network as early as possible. Current Alzheimer's medications can delay the progression of disease with memory symptoms and other cognitive changes.
Two types of drugs are currently used to treat cognitive symptoms:
- Cholinesterase inhibitors : These drugs work by boosting levels of a cell-to-cell communication by providing a neurotransmitter (acetylcholine) that is depleted in the brain by Alzheimer's disease. The improvement is modest. Cholinesterase inhibitors can improve neuropsychiatric symptoms, such as agitation or depression, as well
- Memantine : This drug works in another brain cell communication network and slows the progression of symptoms with moderate to severe Alzheimer's disease. It's sometimes used in combination with a cholinesterase inhibitor.
Sometimes other medications such as antidepressants are used to help control the behavioral symptoms associated with Alzheimer's disease. But some medications should only be used with great caution. For example, some common sleep medications like zolpidem , eszopiclone etc.- may increase confusion and the risk of falls. Anti-anxiety medications such as clonazepam and lorazepam - increase the risk of falls, confusion and dizziness.
As the exact cause of Alzheimer's disease is still unknown, there's no certain way to prevent the condition. But Promising research shows that a person can reduce the risk of Alzheimer’s disease through a combination of simple but effective lifestyle changes.
- Regular exercise is an important part of everybody's wellness plan — and those with Alzheimer's are no exception. Activities such as a daily walk can help improve mood and maintain the health of joints, muscles and the heart. Exercise can also promote restful sleep and prevent constipation.
- People with Alzheimer's may forget to eat, lose interest in preparing meals or not eat a healthy combination of foods. They may also forget to drink enough, leading to dehydration and constipation. So, high-calorie, healthy shakes and smoothies, milkshakes with protein powders can require to make smoothies featuring. Try to ensure that a person with Alzheimer's drinks at least several full glasses of liquids (water, juice and other healthy beverages) every day.
- Avoid beverages with caffeine, which can increase restlessness, interfere with sleep and trigger a frequent need to urinate.
- Cardiovascular disease has been linked with an increased risk of Alzheimer's disease.
- Social interactions and activities can support the abilities and skills that are preserved. Doing things that are meaningful and enjoyable are important for the overall well-being of a person with Alzheimer's disease. These might include listening to music or dancing, reading or listening to books, gardening or crafts, social events at senior or memory care centers and planned activities with children etc.
The latest research suggests that some factor like haring-lose, untreated depression, loneliness, social isolation, sedentary lifestyle, smoking, high alcohol beverage, unhealthy food consume, lazy lifestyle may provoke Alzheimer’s disease.